Jones Fracture

What is it?
A stress fracture is an overuse injury of the bone. A bone will break or fracture when a stress placed on the bone exceeds its ability to withstand stress. A typical break or fracture will occur when an abnormally high force is applied to a normal bone. Stress fractures also occur due to a normal force being applied to the bone an excessive number of times with insufficient rest. Bones are constantly changing and responding to the workload placed upon them. There is a constant turnover of cells as the bone acts to repair itself. When the stress of repetitive loads overwhelms the ability of the bone to repair itself, small cracks will occur – this is otherwise known as a stress fracture. The metatarsals or the long bones in the foot are the second most common place to get a stress fracture. The fifth metatarsal in particular is a very high risk bone and heals very slowly. It has a very high risk of not healing at all. It should be treated with more care than other injuries. See figure 1 and 2 below.
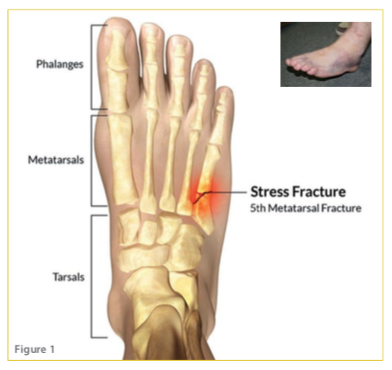
How did I get it?
Stress fractures of the metatarsals can occur due to a multitude of factors. Unstable foot mechanics and excessive loading of the bone are the two most common elements of this injury. Bones are very resilient but force can add up quickly. When running, the force that will travel through the foot is often 3-4 times that of your body weight and when jumping the force can be as high as 10-12 times bodyweight. If there is an abnormal, rather than even, distribution of force due to altered biomechanics the degree of loading force is compounded further. Other factors that may contribute to a stress fracture include changes in training load and / or frequency, training surfaces, footwear, biomechanical abnormalities e.g. having a long second toe or flat feet and muscle tightness or fatigue. Disturbances in a female’s menstrual cycle may also be a contributing factor. Tight constrictive footwear or elevated heels may increase the workload and stress on the metatarsal bones. Such causative factors must be effectively addressed or injury will recur.
What are the symptoms?
A stress fracture of the 5th metatarsal is characterised by increasing pain over the outside of the foot. It usually develops over a period of weeks although sometimes comes on suddenly. The pain is generally very localised over the site of the stress fracture and made worse by exercise. Initially, it may have only been present following activity however with continued loading and stress, the pain may have progressed to be present during exercise. It may also have reached a level such that activity is too painful to perform and the foot is sore during walking, rest and even at night. The site of the pain will be tender.
What should I do?
If you have or suspect you have a stress fracture you should avoid performing weight bearing activity on the “suspect” foot. Avoiding tight shoes and high heels which will place extra stress on the forefoot is also important. The management of stress fractures must be appropriate or there can be long term problems. Inappropriate management of a stress fracture can, at the very least, result in long-term pain – while non-union (the bone not healing together) and osteonecrosis (bone death) are two of the more severe possibilities that can occur due to poor treatment. Surgery may be required. It is important not to forget that even once the fracture has healed sometimes long term training modifications need to occur. Sometimes it is as simple as using an orthotic to correct a biomechanical abnormality but in other cases may involve close attention to your training load and dietary factors etc.

How is a diagnosis made?
A diagnosis is made on the history of the injury and on examination findings. Imaging studies such as x-ray, bone scan or CT/MRI may be used to confirm the diagnosis.
What does rehab involve?
PHASE 1
Day to day activity: Weight-bear as tolerated. For occupations with significant walking/ weight-bearing a walking boot may be required. Limit unnecessary walking.
Exercise:
Yes: Swimming, upper body weight training, grinder.
No: Walking, running, cycling, rowing, elliptical, anything with weight bearing
Sample exercise session for an endurance athlete:
- Swimming preferably with pull buoy to limit kicking
- Intervals on the grinder
- High rep no rest circuit of upper body weights.
PHASE 2
Day to day activity: Weight-bear as tolerated. For occupations with significant walking/ weight-bearing a walking boot may be required. Limit unnecessary walking.
Exercise:
Yes: Swimming, upper body weight training, cycling
No: Walking, running, rowing
Sample exercise session for an endurance athlete:
As previous plus add in cycling. Should aim to be performing a spin class by the end of week 4.
Remember just because you can add in some cycling doesn’t mean that you should be cranking high resistance 7 days per week. It should be added in to slowly and progressively increase the load and provide some variety.
PHASE 3
Day to day activity: Weight-bear as tolerated.
Exercise:
Yes: Swimming, upper body weight training, cycling, rowing
No: Walking, running.
Sample exercise session for an endurance athlete:
As per previous plus rowing.
Sample rowing targets aim for 2500m in 10 minutes.
1min row with 1 minute of rest. 10 intervals of 280m per minute, 2000m in the shortest time possible. Concept 2 have a VO2 max calculator and well established records which you can test yourself against!
http://www.concept2.com/us/interactive/ calculators/vo2max.asp
PHASE 4
Day to day activity: Weight-bear as tolerated.
Exercise:
Yes: Swimming, upper body weight training, cycling, rowing, low volume of jogging on grass
No: running
Sample exercise session for an endurance athlete:
Trial of 4 x 500m jog on grass 3 times over the 2 weeks separated by at least 2-3 days
PHASE 5
PODIATRY REVIEW WITH TREADMILL RUN TO ASSESS BIOMECHANICS
Day to day activity:
Weight-bear as tolerated.
Exercise:
Yes: EVERYTHING, be sensible with loading. Very slow increase in running volume.
Week 1: 2km run 3 times per week
Exogen:
Exogen is a form of Low Intensity Pulsed Ultrasound (LIPUS) which has been shown to accelerate bone healing. It needs to be applied daily, as close to the same time every day as possible. There is free use of exogen at Sports Clinic NQ 5-6 days per week depending on opening hours. Figure 3 provides an example of the device.
Alter G:
Sports Clinic NQ has the only publically available ALTER G treadmill in Queensland, previously only available to professional athletes and members of the armed forces. The ALTER G treadmill, see figure 4, allows you to run at, as little as 20%
of your bodyweight. This provides the following benefits:-
- sport specific conditioning
- graded return to running
- appropriate bone loading to assist the healing process.

